The Quiet Revolution Wrapped Around Your Wrist
Remember the old household arsenal for a quick check-up? A mercury thermometer that took three minutes under the tongue, or a clunky bathroom scale whose needle wobbled between guilt and pride. Today, that once-static snapshot has been replaced by an unblinking, twenty-four-hour documentary—filmed entirely by the watch on your wrist.
What Modern Wearables Actually See
- Pulse signatures: Second-by-second heart-rate plots, down to the skipped beat you didn’t notice while opening your email.
- Arrhythmia whispers: Pattern-finding algorithms scan for atrial fibrillation and raise an on-screen flag before symptoms feel real.
- Blood oxygen in the dark: While you dream, the diodes on your smartwatch measure how efficiently your red blood cells are boarding oxygen at altitude—or after an extra glass of wine.
- Sound bodyguard: Microphones tally decibel levels at concerts, cafés, and subway platforms, suggesting an escape route before your ears file a complaint.
- Soap-opera monitor: Motion and audio cues detect vigorous scrubbing, nudging the owner if the suggested twenty-second birthday song gets chopped into a five-second chorus.
All of these micro-insights are not merely displayed; they’re analyzed, compared, and translated into gentle push notifications on the phone sitting silent on the nightstand. The thermometer now lives in nostalgia’s drawer, while a galaxy of invisible sensors keeps continuous, unobtrusive watch—one heartbeat at a time.
The Apple Watch as Your Silent Health Partner
An afternoon demonstration inside Apple’s campus showed the gadget’s growing role as a pocket-sized clinic. Dr. Sumbul Desai, who heads clinical and health initiatives for the tech giant, ran reporter David Pogue through three features that turn a watch into a lifesaving companion.
Three Ways One Watch Looks After You
- Sound Guardian – The microphone listens, not for words, but for spikes past 85 decibels. A gentle tap on your wrist says “lower the volume or move away.”
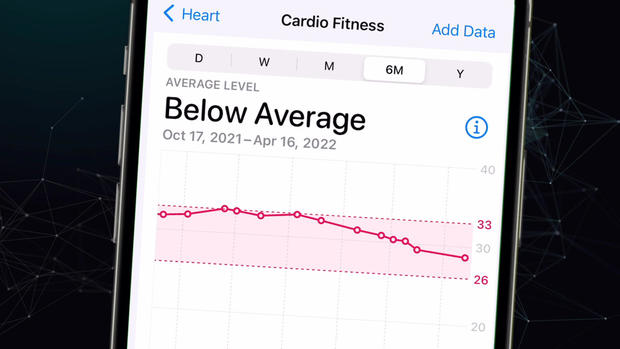
- Cardio Scorecard – VO₂ max estimates arrive every week so you learn, not guess, how your heart and lungs are holding up.
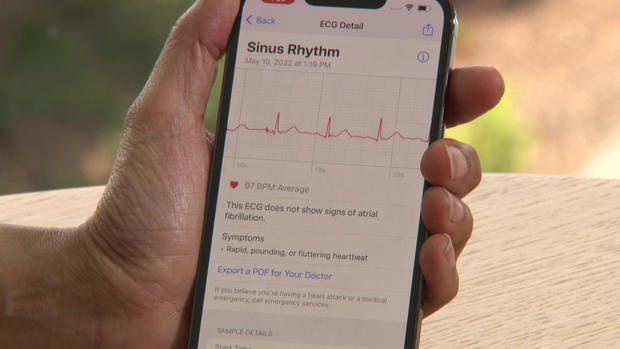
- One-Minute ECG – Rest a finger on the Digital Crown for 30 seconds and the rhythm trace appears. Atrial fibrillation or normal beats are labelled instantly.
From Wrist to Doctor in Two Taps
Once the ECG is complete, users tap “Export to PDF.” A formatted medical report is generated and can be emailed, messaged, or uploaded to a patient portal—no wires, no waiting room forms. “When the data is easy to share, the conversation with your physician starts on day one,” Desai said, handing the generated file to Pogue like a boarding pass to better health.
The Quiet Revolution on Your Wrist: How Next-Gen Smartwatches Are Spotting Trouble Before Doctors Can
From Fitness Tracker to Guardian Angel
Until now, smartwatches were praised for counting steps or logging workouts. The newest models, however, are pushing far past that turf and into the far more dramatic arena of early medical warning. “When your nightly sleep shrinks—or balloons—compared with your own norm, or when your resting pulse settles at an unfamiliar baseline, the device already senses the shift,” notes cardiologist Dr. Manisha Desai.
In plain English: you don’t have to remember to look for signs of trouble; the watch brings the signs to you.
What Gets Flagged Automatically
- Sleep inconsistency—shorter or longer patterns that depart from personal history
- Heart-rate drift—a resting pulse that migrates and won’t return to its usual zone
- Unsteady gait—changes in the way you walk that might predict falls weeks in advance
- Atrial fibrillation (AFib)—a fleeting, often silent quiver of the upper chambers that raises stroke risk six-fold
Why AFib Is the Feature to Remember
Atrial fibrillation turns the heart’s metronome beat into a chaotic tremor. Roughly six million Americans live with it, many without knowing, because episodes can be so brief that a routine office EKG might never catch them. Because the watch stays on your wrist 24/7, it captures the electrical dance when your physician isn’t around.
Whenever the optical sensors spot a skipped or erratic rhythm, the moment is logged and a discreet haptic tap on the wrist arrives asking, “Was this normal for you?” A single tap later, you’ve shared an invaluable clue with your physician days or even months sooner than traditional diagnostics would allow.
What Happens Next
- The watch records a mini-ECG.
- The data syncs to the paired phone.
- A summary appears in the health app.
- You can forward a PDF report straight to your clinic.
The Bottom Line
The newest wrist-hugging devices are no longer just accessories—they are silent sentinels studying every heartbeat, every step, every shift in sleep. The goal is simple and profound: catch problems in the whisper stage, long before they become emergencies.

How a Smartwatch Became Dr. Snyder’s Most Trusted Consultant
A Stanford trailblazer who usually spends his days in the lab has a new hero: the wearable band strapped to his wrist.
Real-Time Insights, Real-World Rescues
Has the data ever made the difference between life and death?
From Odometers to Organ Signals
Michael Snyder, professor at the Stanford School of Medicine, argues it’s time to borrow the dashboard idea from cars and strap it on human bodies.
• We drive vehicles covered in sensors to avoid breakdowns.
• We mostly ignore biological red flags until pain forces us to the clinic.
A Fast-Expanding Diagnostic Radar
Ask Snyder how wide the watch’s medical net might stretch and he rattles off a list that keeps growing:
One Flight, Four False Negatives
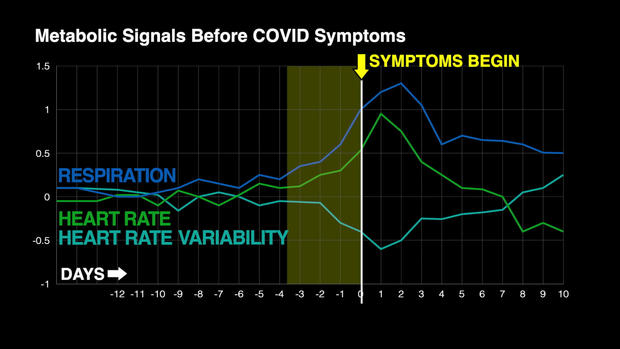
During a cross-country hop last month, Snyder felt stuffed up. His research app pinged him about abrupt shifts in both respiration and pulse.
Mistake. Thirty-six hours later symptoms exploded; PCR confirmed infection. The watch had been three days ahead of every human clue.
100,000 Wrists, Same Pattern
Fitbit’s ongoing study backs the anecdote: in more than one hundred thousand users, measurable metabolic drift tipped researchers off an average of 72 hours before cough, fever, or fatigue arrived. That silent advance warning may soon give airlines, classrooms, and offices time to act before the virus does.
A Health App That Knows You’re Stressed—Though It Hasn’t Figured Out Why
Researchers are edging closer to a future where an algorithm on your phone spots sickness before you feel ill. Right now the most ambitious prototype—led by Stanford geneticist Michael Snyder—watches your heart rate, skin temperature and blood oxygen around the clock. When any one of those numbers spikes in an unusual way, the app fires off an alert. What the alert doesn’t yet say is whether you’re simply grinding through a brutal deadline, coping with a family crisis, or actually fighting off the first phase of COVID-19.
Data, Yes; Context, Not Yet
- Continuous streaming: The app ingests millions of data points each month from off-the-shelf wearables.
- Pattern recognition: A machine-learning layer flags deviations that don’t fit your personal baseline.
- Diagnostic blind spot: Psychological stress, over-training in the gym and sub-clinical viral illness often look identical in the raw vitals.
“We know something is wrong,” Snyder concedes, “but isolating what triggered it is the next frontier.” His team is now recruiting volunteers who agree to log mood surveys, commute times and meal schedules in parallel with the physical data, hoping that richer context will crack the code.
The Voice of Cautious Optimism
Gina Neff, a digital-society scholar at the University of Cambridge and co-author of the acclaimed Self-Tracking, applauds the effort—while sounding a measured note of caution.
“Wearable-driven early warnings could revolutionise preventive medicine, but only if developers solve two problems: cutting down false alarms and protecting the intimate trail of data these devices leave behind.” — Dr. Neff
The Road Ahead
Snyder’s roadmap over the next 24 months includes:
- Folding in hormonal markers such as cortisol to differentiate mental stress from infections.
- Running a joint pilot with a public-health department that routes app alerts into a clinician dashboard for high-risk populations.
- Launching an “explainable AI” feature that shows users exactly which physiological signals triggered their warning so they can learn to respond faster.
If the strategy pays off, your Fitbit or Apple Watch may soon do more than count steps—it could become a personalized early-warning radar tuned to both your stress levels and your risk of the next virus that sweeps the globe.
![]()
The Bright Side of Self-Tracking: Smiles in the Data Stream
The numbers, it turns out, come with a grin tucked inside. Self-monitoring does more than log heartbeats—it builds bridges between people. Those who count steps, minutes of REM sleep, or resting heart rates are, on average, more networked with friends and family. Stronger connections mirror higher self-reported happiness, a finding that MIT researcher Gina Neff calls “the social glue hidden under the metrics.”
Three Feel-Good Outcomes From Everyday Wearables
When Gadgets Watch You Back: The Uneasy Bargain
For all the cheer, a darker subplot lurks. If sensors can praise, they can also judge. Wearable devices designed to “optimize safety” already measure a warehouse picker’s every stride. Miss the speed quota and a badge vibrates—or worse, it quietly informs the shift manager. A telematics box that promises safer driving can secretly relay harsh braking patterns to an insurer, nudging premiums skyward. As Neff warns, “The same sensor that cheers you on can issue a demerit behind your back.”
Red-Flag Scenarios Already in the Wild
Behind the Firewall: What Big Tech Really Sees
Apple’s stance is unequivocal: Nothing leaves your wrist unless you say so. Dr. Sumbul Desai, Stanford’s Vice Chair of Medicine, confirms, “Health data is encrypted on the watch, encrypted on the phone, and encrypted in iCloud—Apple can’t decode it.” In other words, not even the most curious engineer at Cupertino can peek at David Pogue’s blood oxygen trend.
Similar walls exist at Fitbit. Raw biometric details stream first to the user, second (with explicit consent) to chosen apps, and never, according to the company, to marketing teams prowling for ad fodder.
The View From Stanford’s Research Labs
To Michael Snyder, mapping sickness before it strikes is worth the risk calculus. The math is staggering: 3.8 billion people already carry a smartphone; add a $50 smartwatch and global vitals monitoring becomes democratic. He envisions a planet where a wrist ping warns of an oncoming fever before you sneeze.
Snyder’s Three-Step Vision
How to Join the Movement
Stanford Healthcare Innovation Lab is recruiting for its Infectious Disease & COVID-19 Wearables Study. Eligibility is simple: be human, own a wrist, and breathe. Participants pledge to let researchers look—but the mirror faces outward toward illness patterns, never inward toward personal secrets. Enrollment details live on the lab’s site.
Smart Reads for Curious Minds
For deeper context, “Self-Tracking” by Gina Neff and Dawn Nafus (MIT Press Essential Knowledge Series) is available in trade paperback, e-book, and audio formats from Amazon, Barnes & Noble, and IndieBound. It parses the exhilaration and the anxiety that ride along on every heartbeat dataset.
This narrative originated in interviews led by Amol Mhatre; Mike Levine edited for precision.




